Last Updated on October 3, 2023
General Overview:
Discover how Practice Ready Ontario is revolutionizing healthcare access in high-need communities by tapping into the potential of internationally trained family physicians and general practitioners. This innovative 12-week clinical field assessment program, hosted at designated sites, offers a dynamic pathway to address healthcare shortages. Here, candidates undergo a rigorous evaluation of their clinical and non-clinical skills, closely supervised by experienced physician assessors. It’s not about training; it’s about a supervised assessment that paves the way for candidate success. The outcomes of this assessment period are meticulously reviewed by the Practice Ready Ontario Assessment Committee, ensuring that only the most qualified individuals move forward.
But that’s not all – after successfully completing the clinical field assessment, the Ontario Ministry of Health mandates a minimum three-year commitment as family physicians in communities with a Rurality Index for Ontario (RIO) score of 40 and above, or within Northern Urban Referral Centres like Timmins, North Bay, Sudbury, Sault Ste. Marie, and Thunder Bay. To create an authentic assessment environment, we align the clinical field assessments with each candidate’s agreed-upon return-of-service community. Practice Ready Ontario is not just a program; it’s a transformative journey that empowers healthcare professionals to make a lasting impact where it matters most.

Exploring the Commitment: Return of Service with Practice Ready Ontario
In a mission to bolster the presence of family physicians in underserved communities across Ontario, Practice Ready Ontario (PRO) is setting the stage for a transformative journey. A crucial aspect of this journey is the “return of service,” a commitment that carries immense significance in our program.
The Ontario Ministry of Health mandates that all successful candidates in PRO embark on a minimum three-year return of service as family physicians within a government-identified area. This commitment binds candidates to serve in the same Ontario community where they secured their employment offer, aligning their professional dedication with our collective goal of enhancing healthcare access.
Before embarking on their clinical field assessment, candidates sign a return of service agreement with the Ontario Ministry of Health. This contract solidifies their commitment to three years of full-time service as family physicians upon successful assessment completion.
However, it’s important to note that candidates won’t be continuing their service in the same practice where they underwent assessment. Instead, they will be matched with another community sharing a similar profile and demographics, ensuring a well-rounded experience.
The Ontario Ministry of Health has pinpointed eligible practice locations for the return of service commitment, including communities with a Rurality Index of Ontario (RIO) score of 40 and above, as well as Northern Urban Referral Centres such as Timmins, North Bay, Sudbury, Sault Ste. Marie, and Thunder Bay. RIO scores are determined by factors like population, travel times to referral centers, and more.
For transparency, candidates with pre-existing return of service obligations must disclose them during the application process. Furthermore, it’s worth noting that candidates cannot simultaneously participate in both the International Medical Graduate Training return of service program and Practice Ready Ontario.
The return of service commitment is a cornerstone of our program, ensuring that healthcare professionals make a meaningful and lasting impact in the communities where they are needed most. With PRO, we’re not just shaping careers; we’re transforming healthcare access for the better. For a comprehensive look at community RIO scores, please visit the linked site provided.
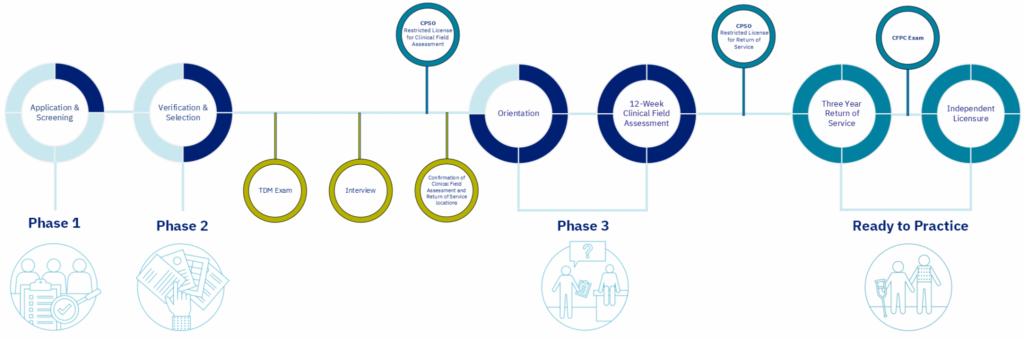
Understanding the Phases
Phase 1: Application and Screening
Applications will be completed through the Practice Ready Ontario Application Portal. At this phase, applicants confirm their eligibility, and share documentation with program administrators through physiciansapply.ca.

Phase 2: Verification and Selection
Eligible candidates who are chosen to proceed to Phase 2 will receive an invitation by email to complete the Phase 2 application form in the portal. During this part of the process the applicant’s credentials will be verified by the program administrators. They will also write the Therapeutics Decision-Making Examination, interview and apply for a restricted license through the CPSO.
Phase 3: Clinical Field Assessment
Candidates who are chosen to proceed to Phase 3 will work under the direct supervision of experienced physician assessors who will observe, assess and provide feedback on the candidate’s clinical and non-clinical skills that relate to family medicine. Over the course of the twelve-week clinical field assessment, candidates should experience a broad range of patient presentations that are common to family practice, including emergency practice. They will need to demonstrate throughout that they have the required competencies for independent practice as a family physician in Ontario.
Types of Questions Asked in an MMI Interview for PRO
Explore the Varied Facets of MMI Interview Questions:
- Ethical Dilemmas: In this segment, you’ll encounter thought-provoking scenarios demanding intricate ethical decisions. As an applicant, your task is to delve into diverse perspectives, weigh the consequences, and propose a meticulously reasoned ethical solution.
- Communication Scenarios: This dimension assesses your interpersonal prowess and your knack for effective communication. Expect scenarios that require you to exhibit empathy, active listening, and articulate communication. These scenarios might include delivering tough news to a patient or resolving team conflicts with finesse.
- Critical Thinking Questions: Brace yourself for challenges that test your quick thinking and analytical skills. These questions may encompass problem-solving tasks, case studies, or intricate situations demanding you to dissect information, factor in multiple variables, and devise a logical solution.
To ace these questions, remember to invest time in comprehending the prompts thoroughly. Explore diverse viewpoints, don’t hesitate to seek clarifications if needed, and then furnish a robustly supported response. Your success in an MMI interview hinges on showcasing ethical acumen, effective communication, and sound judgment. For optimal preparedness, engage in mock interviews and acquaint yourself with common ethical dilemmas and critical thinking exercises. This comprehensive approach will empower you to tackle the diverse challenges that the MMI interview landscape offers.
Credentials Matter: Independent Practice for Aspiring Family Physicians
In the pursuit of becoming a part of Ontario’s healthcare landscape, aspiring family physicians and general practitioners should take note of the vital requirement of having a minimum of three consecutive years of independent practice in their professional journey. This prerequisite serves as a testament to one’s ability to act as a Most Responsible Physician, where you hold the reins in diagnosing, implementing, managing, and overseeing patient treatment plans, along with the authority to prescribe medications and order diagnostic procedures.
When evaluating candidates, preference is given to those with recent independent practice experience, especially those with minimal interruptions or gaps in their work history. So, what exactly constitutes independent practice?
Independent practice is defined as actively serving as an autonomous family physician or general practitioner, functioning as the Most Responsible Physician. In this role, you play a pivotal part in patients’ healthcare journeys, making critical decisions and ensuring their well-being. It’s a role that demands not just medical expertise but also a deep sense of responsibility.
However, it’s important to note that not all work arrangements qualify as independent practice. Volunteer positions, for instance, are considered ineligible if the physician does not hold the Most Responsible Physician role. Similarly, roles involving assistance, observation, or preceptorships do not meet the criteria for independent practice.
As you embark on your path to becoming a valued member of Ontario’s healthcare community, keep these essential guidelines in mind. Independent practice is more than just a requirement; it’s a testament to your ability to provide quality care and make a significant impact in the lives of your patients.
Source: https://touchstoneinstitute.ca/assessment/practice-ready-ontario/#phase-2

